- Direct primary care gives employees direct access to a primary care physician through a flat monthly membership model.
- Employers often use DPC to improve access, strengthen prevention, and reduce avoidable healthcare utilization.
- Traditional DPC can be harder to scale across large or distributed workforces.
- Advanced primary care expands on the DPC model with team-based care, behavioral health integration, and broader access.
Healthcare costs continue to rise, and employers are under pressure to offer better benefits while managing spend responsibly. At the same time, employees expect care that is easier to access, more connected, and built around real life.
That has made primary care strategy a bigger decision for HR leaders, benefits teams, and health plans.
Direct primary care is one model getting increased attention. It offers a more direct relationship between employees and physicians, often with simpler pricing and easier access. But as employers compare options, many are also looking at broader models designed for more complex workforce needs.
This guide explains how direct primary care works for employers, where it can add value, where it may fall short, and how advanced primary care compares.
What Is Direct Primary Care?
Direct primary care (DPC) is a healthcare model where patients, or their employer, pay a flat monthly fee for access to primary care services. Instead of billing insurance for every visit, the model focuses on ongoing care access and a direct physician relationship.
Most DPC arrangements include:
- Preventive care
- Sick visits
- Chronic condition management
- Same-day or next-day appointments
- Direct communication by phone, text, or video
- Basic labs or discounted medications
At its core, direct primary care is built around a 1:1 physician-patient relationship. Employees often work with the same doctor over time, which can improve continuity and trust.
DPC is not a replacement for health insurance. Employers typically pair it with a health plan for hospital care, specialist services, emergency care, and other major medical needs.
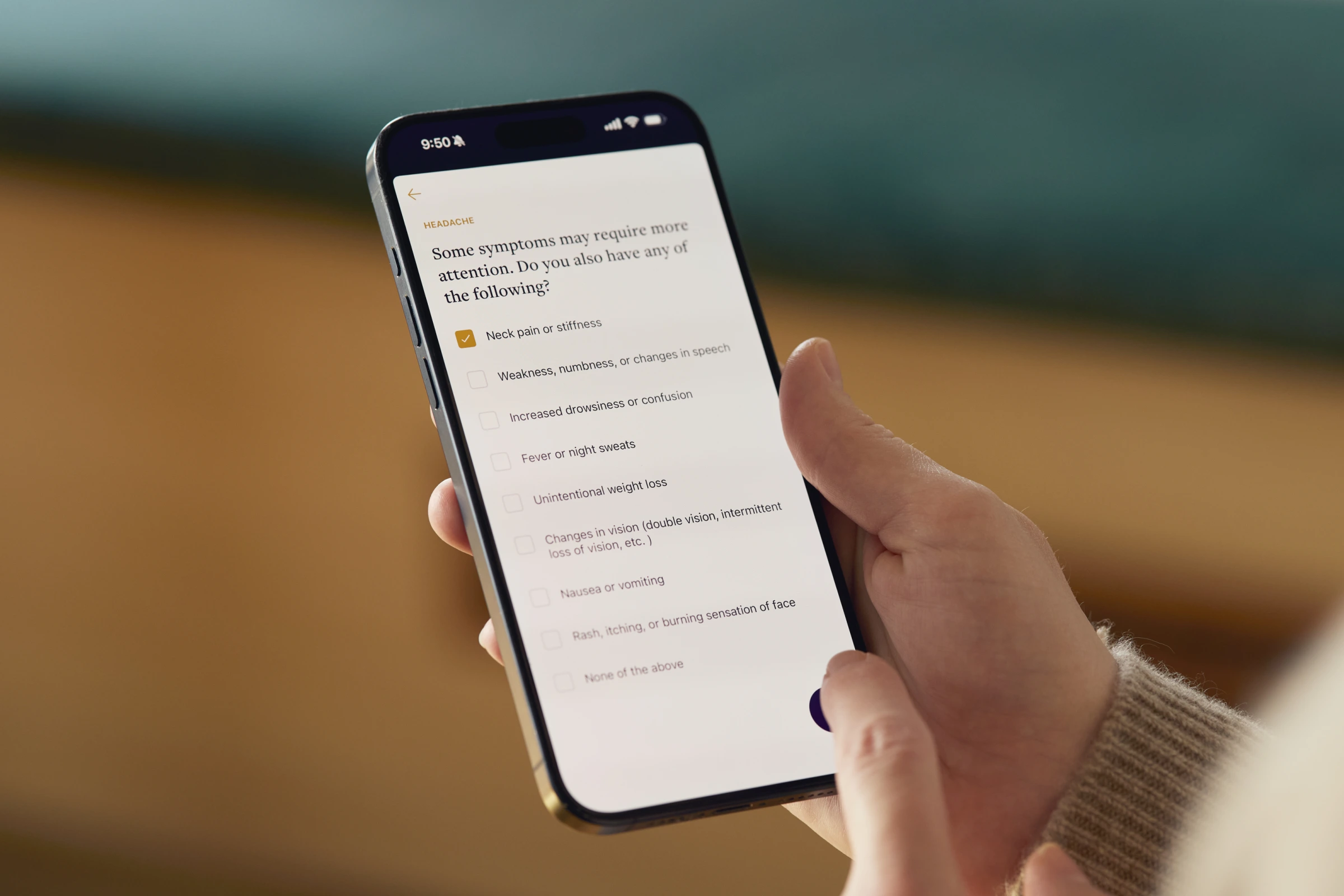
How Does Direct Primary Care Work for Employers?
Employers that offer direct primary care usually contract with a DPC practice or network and pay a monthly membership fee for eligible employees. Typically $50 to $100 per member per month, varying by age and practice. Employees enroll, select a primary care provider, and access care without additional cost at the point of service.
In a typical model:
- The employer sponsors access to the DPC program.
- Employees enroll and select a participating physician or clinic.
- Employees receive covered primary care services with little or no point-of-care cost.
- A separate health plan covers care outside the DPC scope.
This structure can create a simpler care entry point for employees while helping employers encourage preventive and lower-cost care settings.
Direct Primary Care Pros and Cons for Employers
Direct primary care offers employees a membership-based relationship with a primary care physician. Here's what employers should weigh:
Pros:
- Longer, more personalized visits
- Stronger physician-patient relationships
- Predictable, transparent pricing
- Reduced ER and urgent care overuse
- Focus on prevention and chronic condition management
Cons:
- Limited geographic availability
- Requires employees to engage with a local practice
- Not a replacement for insurance (employees still need a health plan)
- Behavioral health is not typically included
- Difficult to scale across distributed or large workforces
The ROI case is real. When employees can reach a provider without co-pay friction, they go earlier and more often. That drives fewer ER visits, lower lab costs through wholesale pricing, and better management of chronic conditions that would otherwise generate expensive downstream claims. The structural cons, however, are built into how traditional DPC is designed; geographic limitations and the absence of behavioral health aren't gaps that a better vendor relationship fixes.
DPC vs. Virtual Primary Care vs. Advanced Primary Care
Employers shopping for a primary care benefit today are navigating three distinct models. The terminology gets used interchangeably, but the differences are meaningful.
Direct primary care is the model described above: a 1:1 physician-patient membership relationship, largely delivered through direct phone and text access, operating outside the traditional insurance system. It works well for employers with geographically concentrated workforces and a willingness to manage the DPC-plus-HDHP structure.
Virtual primary care (VPC) delivers care through digital platforms with 24/7 access. It removes the geography constraint and is well-suited for distributed or remote workforces. The trade-off is continuity: VPC platforms often don't offer the same ongoing relationship with a single provider, and physical examination capabilities are limited.
Advanced primary care (APC) is a team-based model designed for large self-insured employers and health plans. Rather than a 1:1 physician relationship, APC uses multidisciplinary care teams covering a wider range of clinical needs, integrates technology and behavioral health, works within the employer's existing health plan structure, and is built to scale across diverse, distributed workforces.
Here's how the three models compare across the dimensions that matter most for employer benefits decisions:
The right model depends on your workforce profile. DPC's strengths, the personal physician relationship and transparent pricing, are real. But for employers managing large, distributed teams where behavioral health is a growing cost driver, APC offers the same clinical depth with the scale and integration that enterprise benefits require.
What to Ask When Evaluating Direct Primary Care Providers
Before committing to any primary care model, employers should get clear answers on:
- Geographic coverage: Does this practice or network serve all locations where your employees work?
- Panel capacity: Can the practice absorb your employee count while maintaining the access model that makes DPC valuable? The average DPC practice carries around 413 patients, which limits how quickly a single practice can scale.
- Behavioral health: Is mental health care integrated, or are employees on their own for those needs?
- Care coordination: How are specialist referrals and follow-up handled by the practice or by the employee?
- Reporting: Can you access utilization data, ER diversions, visit frequency, and chronic condition engagement to measure ROI?
These are the practical requirements for a model that needs to work across a real, diverse workforce.
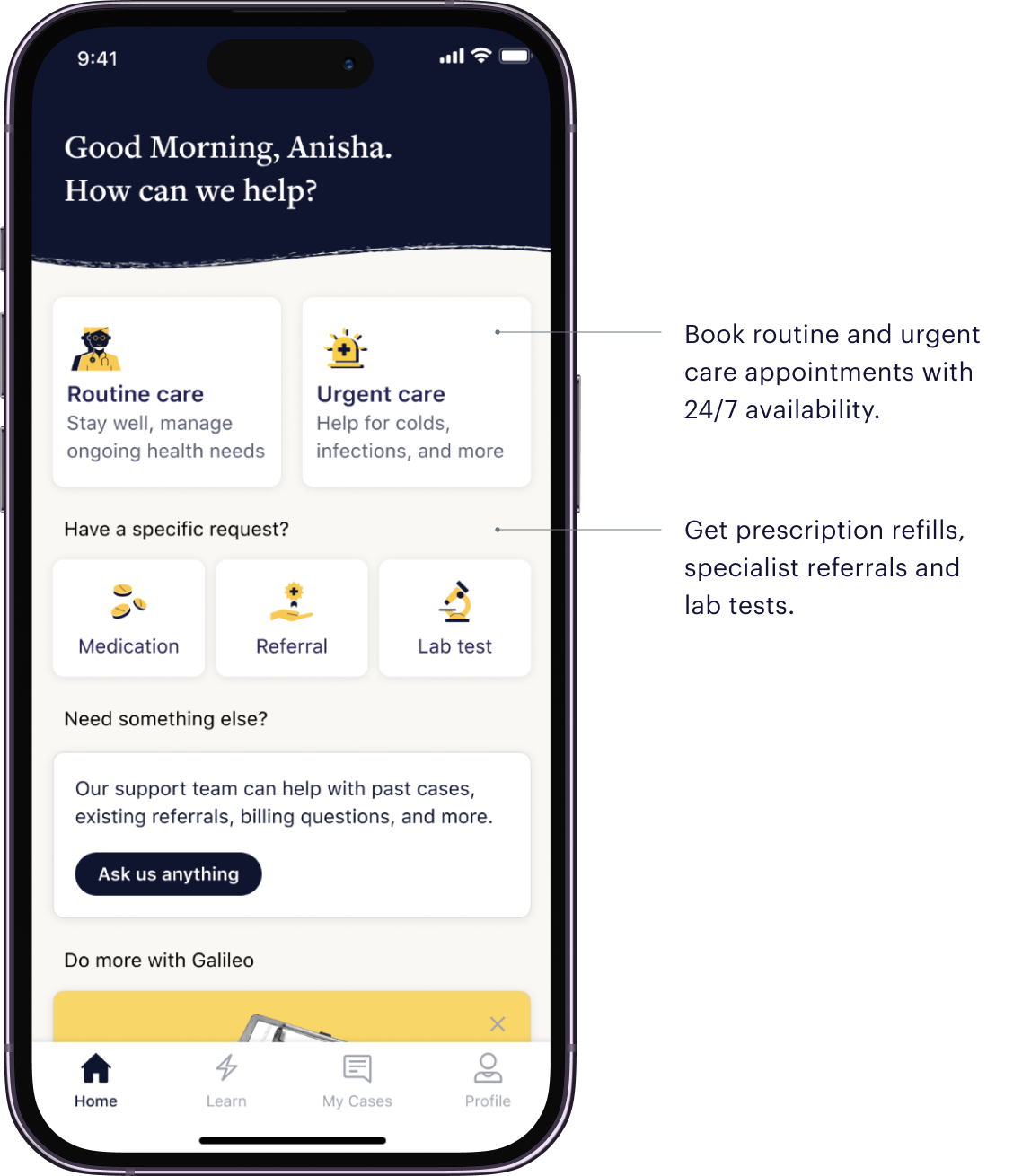
How Galileo Supports Employers
Galileo is built around the same core insight as DPC: when employees have a real primary care relationship, outcomes improve, and unnecessary utilization goes down. Where Galileo operates differently is in how the model is structured to deliver that across a large, distributed workforce.
Galileo is an advanced primary care model. Rather than a 1:1 physician relationship in a local clinic, Galileo uses integrated, multidisciplinary care teams covering 20+ specialties.
More care starts and stays within Galileo across a wider range of clinical needs, rather than fragmenting to specialists or other providers. That longitudinal continuity is what produces the outcomes that drive ROI.
- Available in all 50 states: Galileo's virtual-first model removes the geography constraint entirely. Every employee, regardless of location, has access to the same care.
- In-person and mobile capabilities: For employees in select markets, Galileo also offers in-person and in-home visits, which address one of the core limitations of purely virtual care models while keeping team-based continuity intact.
- Integrated behavioral health: Galileo's care teams include behavioral health support on the platform, so employees can address mental health and primary care needs in the same place without separate referrals. Nearly 75% of mental health patients have a physical comorbidity, treating them through separate benefit silos is both clinically fragmented and more expensive.
- 24/7 access: Employees can reach their care team around the clock. That's what actually reduces ER and urgent care overuse.
- Works within your health plan: Galileo integrates with employers' existing benefits structures and health plan partnerships rather than sitting outside the insurance code. That means less administrative complexity for HR and more continuity for employees.
Is Direct Primary Care Right for Your Workforce?
The answer depends on your employee population and business goals.
Direct primary care may be a strong fit for smaller or geographically concentrated workforces looking for a more personal physician relationship.
Employers with larger, multi-state, or more complex populations may need broader support, including behavioral health integration, national access, and scalable care coordination.
The most effective solution is the one aligned to how your workforce actually lives, works, and uses care.
Primary Care That Performs at Scale
Direct primary care works when the conditions are right. The case for better access to primary care, fewer ER visits, lower lab costs, and more consistent chronic disease management is well established.
But the model has real constraints, including geography, panel size, and limited behavioral health, that matter when you're building benefits for a distributed, diverse workforce.
Advanced primary care addresses those constraints directly: team-based, nationwide, behavioral-health-integrated, and built to work within the health plan structures enterprise employers already use.
If you want to see how a longitudinal, team-based advanced primary care model works in practice, Galileo's team works directly with employers and health plans. Reach out to start the conversation.



%20(1).webp)
%20(1).webp)













.webp)






